About a fifth of the US population which is over 70 million people from all states, use Medicaid public health insurance program. This medical aid program is a lifeline for many low-income Americans. We’ll next get more detailed about the Eligibility terms and all Requirement To Apply For Medicaid
What Is Medicaid
Medicaid is an insurance aid welfare program that is mutually funded by the federal government and the states. It provides health and medical insurance coverage to millions of the neediest eligible citizens of all ages. The program benefits include the coverage of many expensive.
The program includes insurance coverage for many medical health services. Some states may support more services than others. However, in some cases, the citizen may be asked to pay some sort of reduced fees in exchange for some of these additional benefits.
The Social Security Act terms and federal regulations are the main governors to the program requirements and eligibility. The program is available in all states. Even ineligible individuals for Medicaid in certain states can be included in other low-income insurance programs.
We can help get up to $0 monthly premium Medicare plansFind Medicare Plans in 3 Easy Steps
Read More: Three Medicare Surprises No One Told You
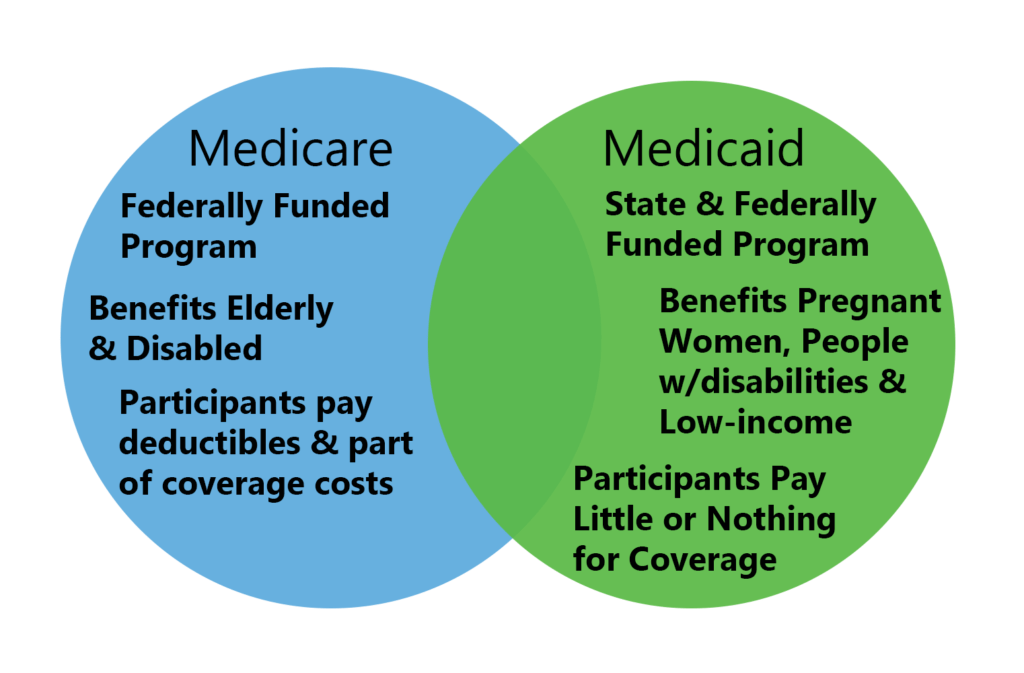
What Is The Difference Between Medicare And Medicaid? And How It’s Different Between Other Plans Like Obamacare
With all the discussions concerning healthcare, ObamaCare, Medicare, and Medicaid, it’s might be confusing for many people to understand the differences between each program. For those who are not up to date on the issue of US healthcare, you can check the table below for a pretty simplified overview:
| Medicaid | Medicare | Obamacare |
About The Program | It’s an aid and assistance program | It’s an insurance program | A private health insurance plan |
The Program Is Managed By | The states and local governments | The Federal Government | Department of Health and Human Services |
Based On | Income | Age | |
Beneficiaries | Low-income individuals | Paying covered senior insured individuals | Individuals earning 400% or less of the federal poverty level |
How Medicaid Work
Once you pass the Medicaid terms of eligibility, you’ll get a medical card and advantages that you can utilize in the same way many may use their private health insurance coverage.
People who qualify for Medicaid usually don’t have to pay a premium for the provided services, yet there are some limitations. In special cases, if an individual is getting Social Security benefits, they may face some sort of reduction from those benefits. Still, it all depends on the amount of their earnings.
Medicaid always acts as the secondary free service provider. This doesn’t imply that you can’t depend on Medicaid benefits. As it will only pay after any other payer has given their portion of the services provided.
If the individual doesn’t have any other sort of insurance coverage, the Medicaid program will give them 100% full and complete coverage for the maximum amount allowed of the provided medical fees. Even Medicaid won’t ask for any premiums or deductibles to be paid in return.
The Reason Behind Medicaid
Before Medicaid was passed, inadequate federal subsidies were delivered to states for health care aids they acquired on behalf of public assistance recipients. In 1960, Congress approved open-ended federal equal amounts to states for the health care rendered to poverty-stricken seniors. However, in the early 1960s, states fluctuated broadly in the range of the health care assortments they supported for low-income groups.
Medicaid was intended to increase admittance to health care services provided for low-income families. The federal government decided then that they would pay for half or even more than half of the costs of the services, Those payments were to be delivered and managed by each state government
Also, the program was prepared to furnish states with a significant degree in creating their own best medical aid plans. States that wanted to engage in the program were obliged to provide proof of the basic services provided to their deserving citizens.
Each participating state was additionally permitted to propose further assistance of their choice and could choose to accept medically needy people who did not get government compensation.
What Is Covered By Medicaid?
All the states have a minimum level of public health services provided within their Medicaid coverage. These services are considered essential, vital, and indispensable to the needy patient they cover. These next medical services are considered necessary and neither Medicaid nor the health care provider will require the patient to pay any copayment in exchange for them.
- Inpatient and outpatient hospital services
- Inpatient short-term skilled nursing or rehabilitation facility care
- Short-term home health care
- Birth control pills and devices
- EPSDT are medical services for early childhood and adolescents such as Early Periodic Screening, Diagnostic, Treatment Services, services from a pediatrician, midwife, or family nurse practitioner, and services at various childbirth medical centers
- Preventive care and immunizations for children under age 21
- Doctor fees
- Laboratory and X-ray services
- Quit-smoking programs
- Ambulance assistance
- Prescription drugs for individuals not included within Medicare
Some states’ Medicaid programs may decide to include more free medical services exceeding the ones above. However, to receive some of the additional services, some states may charge a small percentage of the cost or a copayment. Those extra provided care services are different from one state to another however, they probably include:
- Eye exams and glasses
- Hearing tests and hearing aids
- Dental services
- Preventive x-rays
- Physical therapy (other than the ones listed in Medicare basic services)
- Non-emergency transport costs from and to the medical treatment center
- Additional prescription drugs not included by Medicare
- Some nonprescription drugs, such as vitamins
- Chiropractic care
The Eligibility Of Medicaid And Who Is Eligible For This Federal Program
Qualifying for Medicaid is not at all effortless, and with state-by-state variations, it is not getting any simpler to apply for the program. Get all of the guidance you need from a financial consultant and a competent elder care lawyer before you start the application process to improve your odds of approval.
Medicaid services recipients usually must be residents of the state in which they are applying for Medicaid. All US citizens plus some eligible non-citizens, legal for instance, a level permanent residents. However, some eligibility terms are applied to certain statuses such as age, pregnancy, or parenting.
So, What Are The Requirements To Apply For Medicaid?
Requirement To Apply For Medicaid
In all states, Medicaid renders health coverage for low-income individuals, parents, and children, pregnant ladies, seniors, and the disabled. In few states, the program also includes all low-income adults below a certain income level.
Even though the Medicaid program is federally financed, it is managed at the state level. So each state has its unique assortment of commands and ordinances of this program.
You can use this LINK to find out if you qualify for Medicaid according to your income, household size, and state of residence.
Is There Any Medicaid Application?
Each state has different and more specific instructions on their citizens’ application to the Medicaid program. Just follow your own state’s guidance for presenting your application. Application submission alternatives may include paper forms, online applications, and even in-person applications at your regional Medicaid department.
When you apply for Medicare, you are required to provide the proper certificates and documents to prove your eligibility for the program. For instance, you may need to submit:
- Proof of age
- Proof of citizenship or foreign status.
- Proof of your disability
- Proof of residence
- Proof of all sources of income
- Proof of assets and other resources
- Proof of other insurance
States are obliged to reply to Medicaid regular applications in 45 days. And to respond to disability applications in 90 days.
If your Medicaid application was rejected because it’s missing some data or paperwork, get whatever is required and understand the directions on the rejection letter to resubmit the application. If your Medicaid application isn’t accepted, you are entitled to request an appeal.
Can I Apply For Medicaid Online?
Yes, you can apply for Medicaid through the Health Insurance Marketplace website from HERE then create a Marketplace account and submit your application attached with the required documentation.
Nursing Home
In all 50 states and the District of Columbia, Medicaid will fully pay for nursing home care including all care and room and board to eligible persons. Just note that both the financial conditions and the level of served care vary in every state. Furthermore, Medicaid will pay for long-term nursing home care for however long the person needs that extent for the rest of their life.
Assisted Living
Medicaid assisted living differs by state. This is because Medicaid is partially subsidized by the federal government and partially by the states. It is relevant to understand that Medicaid may not be the most reliable choice to fund assisted living for everyone.
As Medicaid assisted living rates or “reimbursement rates” are not actually that high. That’s why not many assisted living center accepts Medicaid. Also, considering the insufficient scope of provided services, the application requirements, and waiting lists for Medicaid waivers, many people may be better-off obtaining low-cost assisted living outside of the Medicaid program.
We can help get up to $0 monthly premium Medicare plansFind Medicare Plans in 3 Easy Steps
In-home Care
Medicaid does pay for home care for senior individuals. In-home care services are customarily obtainable through your usual state Medicaid plan, however, may also be provided through Home and Community Based Services (HCBS) Medicaid waivers.
Level Of Care Requirements
Nursing Home Level of Care is abbreviated as “NFLOC”. It is a standard of the level of care requirements that must be sufficient for Medicaid nursing home approval. This level of care is also often used as a basis for the individual to receive support and long-term care services from community-based services (HCBS) Medicaid waiver.
Income Eligibility Criteria
- People aging between 19-64 years old with a family income at or below 138% of the Federal Poverty Level (FPL ($17,609 for an individual; $36,156 for a family of four).
- 18 or younger children with a family income at or below 266% of FPL ($69,692 per year for a family of four).
- Pregnant women with a family income at or below 213% of FPL ($36,721 for single pregnant with their first child, $55,806 per year for a family of four).
Asset Requirements
For eligibility requirements of the Medicaid program, each applicant shouldn’t have more than $2,000 in “countable” assets. Married couples with both husband and wife applying are usually allowed to have up to $4,000 in countable assets.
Steps To Apply For Medicaid
- Check if you’re eligible for Medicaid in your state.
- Collect all required information to fill out the Medicaid form.
- Submit your Medicaid application.
The Cost Of Medicaid
For most of the provided Medicaid health care services, you’ll be 100% covered, receiving all the basic services absolutely free of charge. In the case of the additional services provided uniquely by each state, a copayment may be required in exchange for the service. Also, a monthly premium might be proposed under a federal waiver for specific eligibility categories.
Read More:
- Sign up for Medicare part ABC and D
- Which Medicare Advantage Plans Cover Dental Implants?
- What Is Medicare Part A & B | 2021 Full Guide?